AI in Healthcare in India: Opportunities, Risks, and Lessons for the Global South
A case study examining the opportunities, risks, regulations, and ecosystem of AI in healthcare in India.

AI Case Studies from the Global South
Part 1 of 1
Table of Contents
- 🎥 Can AI Fix India’s Healthcare System? Opportunities, Risks, and Startups - Mar 2026 **
- AI in Healthcare in India: Opportunities, Risks, and Lessons for the Global South
- Conclusion
- Related in this cluster
- 📥 AI Case Studies from the Global South: AI in Health - India Story (PDF)
- 💬 Join the Conversation
- 🌍 Follow GlobalSouth.AI
- Subscribe to stay updated on new case studies, frameworks, and Global South perspectives on responsible AI.
🎥 Can AI Fix India’s Healthcare System? Opportunities, Risks, and Startups - Mar 2026 **
AI in Healthcare in India: Opportunities, Risks, and Lessons for the Global South
Executive Summary
Healthcare systems across the world are facing structural strain. Aging populations, rising chronic diseases, and shortages of trained clinicians are creating a widening gap between demand and capacity. Artificial Intelligence (AI) is emerging as a potential force multiplier that can expand screening, diagnostics, monitoring, and operational efficiency.
India presents one of the most important real-world laboratories for understanding the impact of AI in healthcare. With a population exceeding 1.4 billion people, large rural populations, fragmented health records, and a persistent shortage of specialists, traditional healthcare models cannot scale fast enough to meet demand.
This evidence case study examines the AI healthcare ecosystem in India, focusing on:
- structural healthcare constraints
- emerging AI-driven solutions from startups and public infrastructure
- systemic risks such as bias, infrastructure inequality, and cybersecurity
- regulatory frameworks shaping safe adoption
- lessons for other Global South countries deploying AI in healthcare
The central insight is clear:
India does not need AI because it is technologically fashionable. It needs AI because the traditional healthcare model cannot scale to its population needs.
However, AI solutions that succeed in India must be designed for low-resource, high-diversity environments, where connectivity, data quality, workforce capacity, and affordability constraints shape deployment outcomes.
1. The Structural Healthcare Challenge
India’s healthcare challenge is not fundamentally a technology problem. It is a scale problem.
Traditional healthcare expansion relies on increasing the supply of hospitals, specialists, and physical care infrastructure. But training clinicians and building facilities takes years or decades.
Meanwhile, healthcare demand is rising rapidly due to three structural shifts.
1.1 Shortage of Specialists
Community Health Centres (CHCs) form the backbone of rural healthcare in India. In principle, each CHC should include specialists such as:
- surgeon
- physician
- gynecologist
- pediatrician
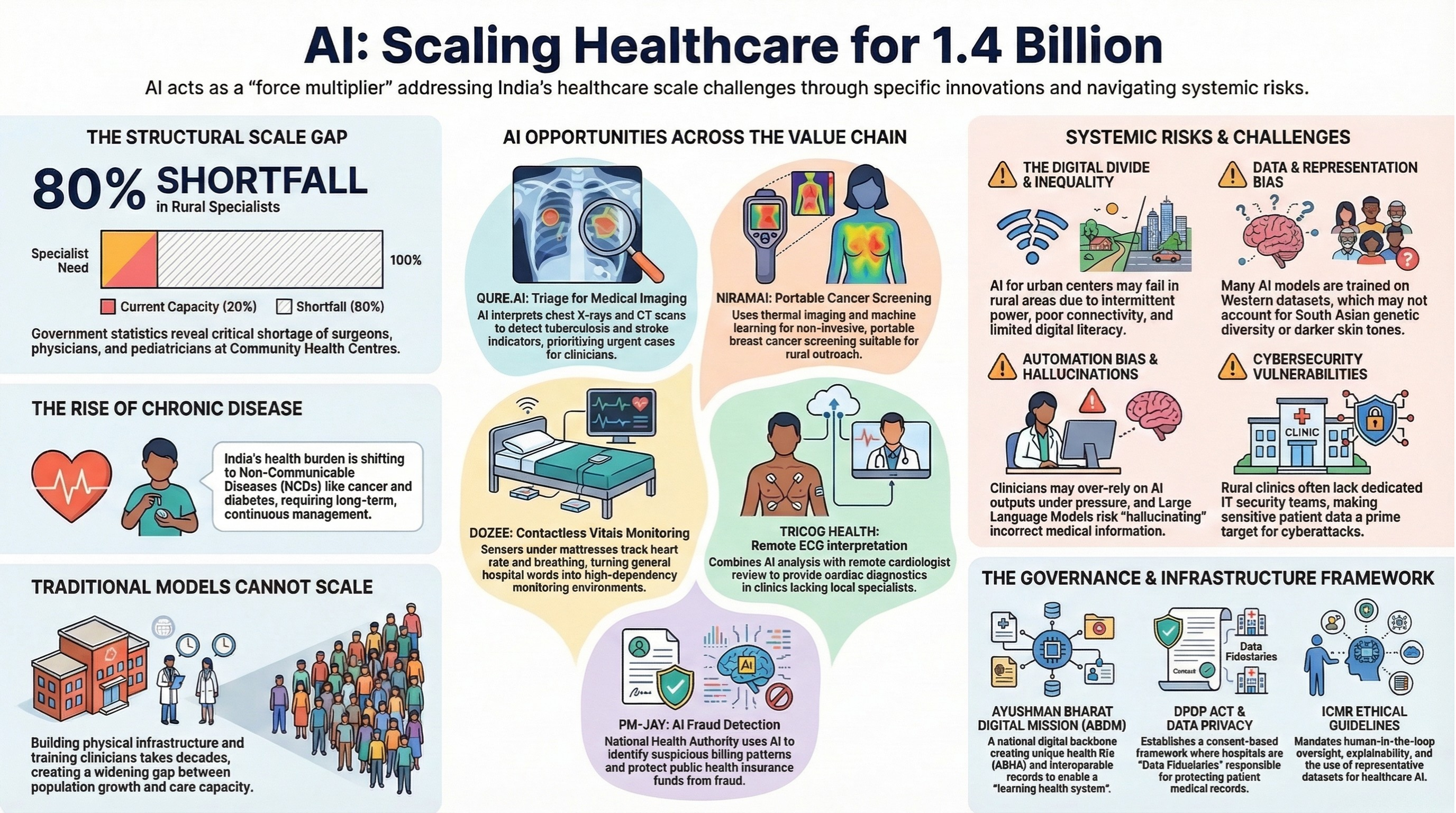
In practice, specialist shortages are severe. Government statistics indicate nearly 80% shortfall in specialist availability at CHCs.
This shortage creates a bottleneck in qualified clinical attention. Patients often delay care, travel long distances, or incur significant out-of-pocket costs in private systems.
1.2 Shift Toward Chronic Disease
Historically, India’s healthcare infrastructure evolved to handle infectious diseases and episodic care. However, the disease burden is shifting toward non-communicable diseases (NCDs) such as:
- diabetes
- cardiovascular disease
- cancer
- chronic respiratory conditions
Chronic diseases require continuous management rather than episodic treatment. They involve long-term monitoring, medication adherence, and early detection of complications.
The traditional healthcare model struggles to provide this level of sustained care at population scale.
1.3 Infrastructure Expansion Cannot Keep Pace
Even with aggressive investment in healthcare infrastructure, scaling physical capacity alone cannot keep up with population growth and rising disease burdens.
This structural gap creates the context in which AI solutions are emerging.
2. AI Opportunities Across the Healthcare Value Chain
AI is increasingly being deployed across multiple points in the healthcare system, particularly where specialist bottlenecks limit access to care.
In India, the most impactful AI applications are not futuristic robotic surgery systems. Instead, they focus on scaling frontline capabilities.
2.1 Screening and Diagnostics
Early diagnosis is one of the most critical leverage points in healthcare. When diseases are detected late, treatment becomes more complex, expensive, and less effective.
Several Indian startups are applying AI to improve diagnostic access.
Qure.ai
Qure.ai develops AI systems for interpreting medical imaging such as chest X-rays and CT scans.
These models detect abnormalities related to tuberculosis, lung disease, and stroke indicators, enabling hospitals to triage urgent cases and reduce delays in diagnosis.
Niramai
Niramai uses machine learning and thermal imaging to support early breast cancer screening.
Unlike traditional mammography, the system is non-invasive and portable, making it suitable for outreach programs and clinics in lower-infrastructure environments.
SigTuple
SigTuple focuses on AI-powered microscopy systems that digitize pathology workflows.
Slides are converted into high-resolution digital images that can be analyzed by AI models, enabling automated anomaly detection and remote specialist review.
AiKenist
AiKenist focuses on improving MRI imaging workflows using AI-based image enhancement and triage systems. The goal is to increase diagnostic throughput using existing imaging infrastructure.
2.2 Remote Monitoring and Precision Medicine
AI is also being applied to continuous patient monitoring and personalized treatment strategies.
Dozee
Dozee has developed a contactless monitoring system placed under hospital mattresses. Sensors detect micro-movements related to heart rate and breathing, enabling early warnings when patient vitals deteriorate.
AarogyaAI
AarogyaAI uses machine learning to predict drug resistance patterns in tuberculosis using genomic sequencing data.
This helps clinicians avoid ineffective treatment regimens and begin appropriate therapy earlier.
Peptris Technologies
Peptris applies AI models to drug discovery, scanning large chemical libraries to identify promising molecules for experimental testing.
This reduces failed experiments and accelerates drug development cycles.
Tricog Health
Tricog operates a distributed ECG interpretation platform that combines AI analysis with remote cardiologist review.
This hub-and-spoke model enables cardiac diagnostics in clinics without local specialists.
2.3 Telemedicine and System Efficiency
AI is also being integrated into digital health infrastructure and healthcare administration.
eSanjeevani
eSanjeevani is India’s national telemedicine platform.
It supports doctor-to-patient and doctor-to-doctor consultations and has processed millions of consultations nationwide.
AI-driven clinical decision support tools are increasingly being integrated into the platform.
PM-JAY Fraud Detection
The National Health Authority uses AI to identify suspicious insurance claims in the Ayushman Bharat PM-JAY scheme.
These models detect billing anomalies and help prevent fraudulent claims, protecting public healthcare funds.
Flabs
Flabs develops generative AI reporting tools for radiology and pathology workflows.
These tools convert clinician dictations into structured reports, improving reporting speed and reducing clinician workload.
3. Risks of AI Deployment in Healthcare
Despite its benefits, AI introduces several risks that may be amplified in the Indian healthcare context.
3.1 Structural Inequality
Two-thirds of India’s population lives in rural areas, but healthcare infrastructure remains concentrated in cities.
AI systems designed for urban hospitals may fail in settings with:
- intermittent internet connectivity
- unreliable power supply
- limited digital literacy
- incomplete electronic health records
Technology often amplifies the capacity of the systems it enters. In low-capacity environments, it can amplify fragility.
3.2 Data Bias and Representation Gaps
Many medical AI models are trained on datasets from North America or Europe.
These datasets may not represent:
- South Asian genetic diversity
- darker skin tones in dermatology datasets
- environmental and dietary differences
Measurement bias also occurs when imaging equipment and diagnostic conditions differ across facilities.
3.3 Human–AI Interaction Risks
Automation bias can occur when clinicians defer to algorithmic outputs under time pressure.
Large language models introduce additional risks, including:
- hallucinated medical content
- fabricated citations
- over-reliance on automated suggestions
Without verification mechanisms, such errors could propagate into clinical decisions.
3.4 Cybersecurity Risks
Healthcare is increasingly targeted by cyberattacks.
Hospitals store sensitive patient data and operate critical systems that must remain continuously available.
Rural facilities often lack dedicated cybersecurity teams, making them particularly vulnerable.
4. Regulatory Frameworks Governing Health AI in India
India is gradually building a regulatory ecosystem to govern AI deployment in healthcare.
Three pillars are shaping adoption.
Data Protection and Privacy
The Digital Personal Data Protection (DPDP) Act establishes a consent-based framework for processing personal data. Hospitals and health technology providers are classified as Data Fiduciaries, responsible for protecting patient data and ensuring lawful processing. Large platforms may be designated Significant Data Fiduciaries, requiring additional obligations such as audits and transparency requirements.
Medical Device Regulation
AI tools that perform diagnostic or clinical functions may be classified as Software as a Medical Device (SaMD). These systems fall under the Central Drugs Standard Control Organization (CDSCO) and must meet risk-based regulatory requirements.
Ethical Guidelines
The Indian Council of Medical Research (ICMR) has issued ethical guidelines for AI in healthcare.
Key principles include:
- human-in-the-loop clinical oversight
- explainability and transparency
- bias mitigation and representative datasets
These guidelines aim to ensure AI systems augment clinicians rather than replace them.
5. The Future of Digital Health in India
India is building a national digital health infrastructure that could significantly shape the future of AI-enabled healthcare.
The Ayushman Bharat Digital Mission (ABDM) includes:
- ABHA (Ayushman Bharat Health Account) IDs enabling unique health identities
- Unified Health Interface (UHI) enabling interoperable healthcare services
- digital health records linked across providers
This infrastructure could enable a learning health system, where data from millions of patient interactions improves diagnostics, treatment protocols, and public health surveillance.
However, the long-term success of this system will depend on whether digital health infrastructure becomes inclusive across both urban and rural populations.
Conclusion
India represents one of the most important testing grounds for scalable AI healthcare systems.
The country combines:
- massive population scale
- diverse health conditions
- infrastructure constraints
- rapidly evolving digital public infrastructure
These conditions make India a valuable case study for other Global South countries deploying AI in healthcare.
The key lesson is that successful health AI systems are not defined by algorithmic sophistication alone.
They must be designed around real-world constraints:
- connectivity limitations
- workforce shortages
- affordability requirements
- diverse patient populations
If AI solutions can operate effectively within these constraints, they may significantly expand healthcare access.
If they cannot, they risk reinforcing existing inequalities.
Related in this cluster
📥 AI Case Studies from the Global South: AI in Health - India Story (PDF)
👉 Download the Case Study Deck (PDF)
🔎 Explore the AI Case Studies from the Global South
Stay tuned — new posts every week!
💬 Join the Conversation
Have thoughts, experiences, or questions about AI fairness? Share your comments, discuss with global experts, and connect with the community:
👉 Reach out via the Contact page
📧 Write to us: [email protected]
🌍 Follow GlobalSouth.AI
Stay connected and join the conversation on AI governance, fairness, safety, and sustainability.
- LinkedIn: https://linkedin.com/company/globalsouthai
- Substack Newsletter: https://newsletter.globalsouth.ai/
Subscribe to stay updated on new case studies, frameworks, and Global South perspectives on responsible AI.
Related Posts

What Anthropic’s AI Jobs Study Misses in the Global South
Anthropic’s recent study on AI and jobs offers valuable insights into how artificial intelligence may affect labor markets in advanced economies. But the same framework does not fully capture how workforce disruption unfolds in the Global South—where informality, youth employment pressures, and service outsourcing shape labor market realities.

The Silent AI Shock in Workforce: An India Case Study
Why unemployment statistics will miss the real disruption of AI in the workforce in the Global South

Access Denied: How India's Digital 'Cure-All' Became a Real-World Fairness Crisis
How Aadhaar’s promise of digital inclusion turned into one of the largest algorithmic exclusion crises in the world.